Industries
With a deep understanding of local conditions, we tackle complex issues from multiple perspectives to deliver innovative solutions
Industries
Energy
Providing advice and forecasts in the area of energy sector investment

We provide expert advice on energy. Principal economics are experts in the field of energy economics with experience in developing and adopting economic models assessing energy issues in New Zealand.
Environment
Fundamental uncertainty in the future climate requires new ways of planning

We offer a comprehensive range of services to support our clients in navigating the complex landscape of climate change and environmental issues. Our team of experts are experienced in conducting literature reviews, policy assessments, and decision making under conditions of fundamental uncertainty
Health
Housing
Housing depends on a range of factors, including affordability, location of jobs and preferences

Our team at Principal Economics encompass a unique combination of knowledge, experience, and skills suited for solving spatial and urban development and housing issues.
Infrastructure
Robust economic frameworks and empirical methods, informed by evidence, shaped in collaboration with stakeholders.

We assist our clients in identifying the primary and secondary impacts of infrastructure investments.
Tourism
Valuing the direct and indirect benefits and costs of tourism

We have used different data sets alongside with our tourism modelling capabilities for evaluating the impact of a range of investments and policy initiatives in the tourism sector.
Regulatory Economics
Transport
Accessibility is the potential for interaction with locations dispersed over space

Our team currently lead some of the most important transport policy topics. This includes providing expert advice on transport equity, emission reduction policies and decision making under deep uncertainty.
Capabilities
Our innovative solutions are tailored carefully to the questions at hand
Capabilities
Economic impact analysis

Making decisions in uncertain times needs precise understanding of the costs and benefits. We can assist by identifying fiscal, economic and wellbeing benefits from your investment decision or policy intervention.
Economic research

Making decisions in uncertain times needs precise understanding of the costs and benefits. We can assist by identifying fiscal, economic and wellbeing benefits from your investment decision or policy intervention.
Market analysis

Making decisions in uncertain times needs precise understanding of the costs and benefits. We can assist by identifying fiscal, economic and social benefits from your investment decision or policy intervention.
Macroeconomic consulting

In the rapidly changing global economy, it is increasingly essential to have a comprehensive understanding of macroeconomic dynamics and conduct a robust analysis of the economic environment to make informed strategic decisions.
Cost benefit analysis

Making decisions in uncertain times needs precise understanding of the costs and benefits. We can assist by identifying fiscal, economic and wellbeing benefits from your investment decision or policy intervention.
Forecasting and modelling

Making decisions in uncertain times needs precise understanding of the costs and benefits. We can assist by identifying fiscal, economic and wellbeing benefits from your investment decision or policy intervention.
Spatial analysis and modelling

In the rapidly changing global economy, it is increasingly essential to have a comprehensive understanding of macroeconomic dynamics and conduct a robust analysis of the economic environment to make informed strategic decisions.
Business case approach

Our team have led business cases for a range of sensitive topics.
About Us
Our consultancy services are driven by the questions of clients, informed by robust evidence, shaped in collaboration with stakeholders, rooted in multi-deciplinary approaches and guided by principles of Economics. Our company is a Tier 2 AOG consultant.
About Us
Our purpose, mission and values

We exist to strengthen economic decision-making in complex systems. Grounded in economic theory and rigorous analytical practice, we apply advanced modelling and disciplined strategic reasoning to support institutions facing high-stakes choices. We integrate emerging analytical tools, including artificial intelligence, where they enhance clarity and evidence — not as substitutes for judgement, but as instruments of deeper economic insight.
Our Corporate Commitments

At Principal Economics, we are dedicated to making a positive impact on society and delivering value to our clients through our unwavering commitment to excellence and responsible business practices. As an economics consulting firm, we recognize the importance of addressing the pressing challenges of our time and striving for inclusive growth, community engagement, diversity and inclusion, ethics and integrity, health and safety, as well as sustainability.
How We Work
Exceptional People and Culture

At Principal Economics, our approach to work is driven by a commitment to excellence, collaboration, and client-centricity. We leverage our expertise, draw inspiration from industry-leading organisations, and continuously refine our practices to ensure we deliver exceptional results. Here's an overview of how we work:
Publications
Our reports offer inspiring and independent insights into various topical issues
Knowledge Hub
Here we provide frontier knowledge and data collected from our latest reports and analyses
Articles
Our articles challenge the status quo by reframing current issues, sparking fresh conversations and finding new solutions
Tools
Artificial Intelligence, Economic and Policy Toolkits
Publications
Knowledge Hub
Articles
Tools
Economic Impact of New Zealand's Second Emission Reduction Plan
CGE modelling of ERP2

This report uses CGE modelling to estimate GDP, employment and distributional impacts of the Emissions Reduction Plan 2 (ERP2), which delineates Aotearoa New Zealand's strategy to attain its emissions reduction objectives for the 2026-2030 period, alongside setting a path towards achieving long-term emissions reduction objectives.
Climate change adaptation and investment decision making

Aotearoa New Zealand suffers from an infrastructure deficit. Without the key infrastructure needed now for our economy to thrive, we deprive future generations from significant economic prosperity.
Review of Housing and Business Development Capacity Assessments

The Ministry for the Environment (MfE) appointed Principal Economics to review the Housing and Business Development Capacity Assessments HBAs). Our review included all councils’ HBAs, except for Rotorua and Wellington, which were not available at the time of this review.
Incorporating distributional impacts (equity) into the CBA framework

Transportation decisions can have large and varied impacts on travellers and their communities. It’s important to measure these effects and consider their impact on various groups when planning projects.
Business Development Capacity Assessment for Dunedin City

Dunedin City Council appointed Principal Economics to provide a comprehensive assessment of the sufficiency in development capacity of business land within Dunedin to fulfils requirements of the the National Policy Statement on Urban Development
See all Publications

Read inspiring publications that challenge conventional thinking by reframing current issues, igniting fresh conversations, and discovering innovative solutions.
Database of road transport elasticities
Emission reduction initiatives

We provide a comprehensive summary of potential policy areas suitable for emissions reduction. This inludes a review of policy areas including active transport, mobility as a service, ridesharing, telework, parking pricing, road user pricing, carbon taxes and more.
VKT Dashboard
This household and regional VKT dashboard showcases the power of using frontier data manipulation methods and granular IDI data
Drivers of House Price Growth

We provide an extensive review and test the factors of housing price growth in New Zealand. We assessed the level of agreement and certainty with the source of house price growth over the last fifty years.
See All Knowledge Hub
SURF
Shaping New Zealand’s Health Adaptation Strategy
Transport equity
See All Articles
Contact Us
Our team
Chief Executive Officer

Eilya is the CEO of Principal Economics with extensive executive and consultancy experience. Eilya is experienced in managing large teams of applied researchers and has led a wide range of high-profile infrastructure projects in New Zealand.
Chris Parker

Chris Parker is a leading applied economist and policy advisor with deep expertise in urban economics, infrastructure, and cost-benefit appraisal.
Our Team

Our team integrates economic theory, advanced modelling, and disciplined strategic reasoning to support consequential decisions. We operate across infrastructure, energy systems, climate transition, and regulatory economics.
Shaping New Zealand’s Health Adaptation Strategy
Principal Economics
Leading the health V&A evidence for the NAP
Our expert team at Principal Economics leads the Ministry of Health’s climate–health Vulnerability and Adaptation (V&A) assessment.
The assessment is a key driver of adaptation strategy because it turns climate change into quantified, place-based health risks and clarifies which interventions reduce harm.
It aligns directly with the health sector’s adaptation direction set out in the Ministry’s Health National Adaptation Plan (HNAP), and it supports the wider National Adaptation Plan (NAP) led by the Ministry for the Environment.
See: Health National Adaptation Plan 2024–2027 and National Adaptation Plan.
We use a decision-grade evidence chain. We start with explicit climate scenarios because scenarios define the risk envelope, timing, and the appropriate adaptation stance.
From scenarios, we map hazard pathways with measurable indicators.
We then link those hazard indicators to granular health risks across communities using condition-specific relative risk matrices.
Finally, we focus on health system capacity as the core instrument for reducing vulnerability—assessed through a social welfare lens that makes economic constraints and equity trade-offs explicit.
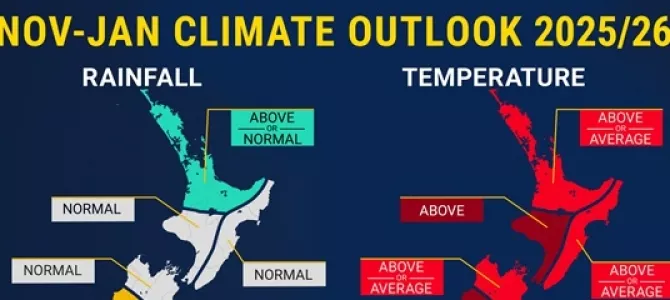

Scenarios anchor adaptation choices
Climate scenarios are not a technical preface. They determine what government is planning for, when impacts emerge, and whether the right response is incremental adjustment or structural change.
Without explicit scenario choices, strategy tends to drift toward median planning (systematically under-preparing) or toward unbounded risk aversion (over-investing without transparency).
Our V&A work therefore starts with scenario selection and uses it to structure the evidence base.
Scenarios define the plausible future conditions that drive hazard frequency, intensity, and duration.
This creates a disciplined basis for prioritisation and sequencing: scenario choices set the envelope for action, and subsequent modelling clarifies which investments remain robust across plausible futures.
Pathways connect climate to health
From scenarios, we map the climate–health pathways that matter for New Zealand.
These include extreme weather injuries and fatalities; heat-related illness and mortality; waterborne and foodborne diseases; vector-borne diseases; respiratory impacts from air quality, wildfire smoke, and allergens; and mental health and wellbeing.
Each pathway specifies (i) the climate driver, (ii) the hazard manifestation relevant to New Zealand, and (iii) the indicator set used to represent it in a measurable and updateable way.
This pathway structure avoids an unprioritised hazard list.
It produces a portfolio that can be compared, stress-tested, and revised as evidence improves.
It also makes policy levers clearer by linking hazards to operationally meaningful metrics that can inform warnings, preparedness planning, and service design.

From evidence chain to strategy
Indicators designed for implementation
Hazard indicators form the interface between climate science, modelling, and policy.
We prioritise indicator sets that agencies can observe historically, project under scenarios, and interpret in operational settings.
Where feasible, we align indicators with the way risks are managed in practice—through thresholds, alerts, standards, and planning assumptions—so the assessment connects directly to intervention design.
This matters for the NAP because monitoring and accountability depend on measurable constructs.
An implementable indicator set allows agencies to (i) define triggers, (ii) target interventions, and (iii) track whether adaptation reduces vulnerability over time.
It also improves transparency by making clear how hazard change is represented and how results would shift under alternative indicator choices.
Relative risk matrices translate evidence
The technical translation step uses condition-specific relative risk matrices: structured mappings from exposure (and where relevant, lagged exposures) to changes in health risk.
These matrices provide the bridge from scenario-driven shifts in hazards to quantified impacts on morbidity and mortality.
They also support comparability across hazards and health conditions by putting results on a common risk footing that can be aggregated, decomposed, and communicated clearly.
We keep the purpose strategic.
Relative risk matrices allow decision-makers to see where marginal risk reduction is likely to be greatest and where targeted investment will deliver the strongest welfare gains.
They also preserve auditability by linking priorities back to the underlying evidence and key assumptions.


Granular community risk, not averages
Adaptation decisions must work where risks manifest and services respond.
National averages conceal clustered vulnerability, compounding disadvantage, and local capacity constraints.
We therefore apply the scenario–hazard–risk chain at fine spatial resolution to identify priority communities and suburbs, rather than only reporting broad regional patterns.
This granularity supports equity-centred planning.
It shows how the same hazard can lead to different impacts depending on baseline health, exposure patterns, socioeconomic conditions, and adaptive capacity.
It also improves validation and learning because local results can be compared with observed service use and outcomes, strengthening confidence in priorities and highlighting where further evidence development is needed.
Health system capacity is the core lever
We place health system capacity at the forefront because it is the primary instrument that turns climate risk into avoidable harm—or preventable resilience.
Exposure may rise under most scenarios, but outcomes depend on prevention, access, quality of care, surge capability, continuity planning, and public health functions.
Capacity therefore operates across hazards and supports actions that remain valuable under multiple futures.
This framing shifts V&A from describing vulnerability to reducing it.
It supports practical adaptation packages such as strengthening primary and preventive care, improving emergency readiness, enhancing surveillance and early warning, protecting continuity of care during extreme events, and targeting underserved areas where welfare gains are largest.
This focus is consistent with the intent of the Ministry’s HNAP to strengthen health-sector readiness and resilience.
Social welfare and economic realism
Capacity decisions require a social welfare lens because adaptation involves real trade-offs under resource constraints.
A welfare framing makes objectives explicit: reduce avoidable morbidity and mortality, protect equity, and maintain system functioning.
It also provides a principled basis to compare interventions that operate through different channels—prevention, service delivery, infrastructure, and community supports.


HVAT operationalises the full chain
Economic considerations are essential to implementation.
Workforce limits, capital budgets, opportunity costs, and distributional impacts determine what can be delivered, sustained, and scaled.
Ignoring these constraints produces strategies that read well but fail in practice.
Embedding economics ensures the V&A assessment supports credible prioritisation and sequencing within the real decision environment of the NAP and HNAP.
All of this is implemented through the HVAT — Health Vulnerability & Adaptation Toolkit.
HVAT operationalises the scenario-to-decision chain: it starts from explicit scenario choices, maps hazards and indicators into pathways, applies condition-specific relative risk matrices to estimate granular impacts, and places health system capacity at the centre as the main adaptation lever assessed through a social welfare and economic lens.
It provides a repeatable framework to prioritise hazards and places, design robust interventions, monitor vulnerability over time, and update evidence as projections and health research evolve.
Concluding remarks
New Zealand’s adaptation strategy needs a clear line of sight from climate futures to health outcomes and to the capacity investments that reduce harm. Our V&A work provides that line of sight by combining scenario-led hazard analysis, evidence-based relative risk translation, granular community impacts, and an explicit focus on health system capacity under a social welfare and economic lens. This approach strengthens prioritisation, supports equity, and improves the implementability and accountability of the NAP.
Links: Ministry of Health HNAP · National Adaptation Plan · HVAT Toolkit

